Journal of Clinical and Experimental Ophthalmology
Open Access
ISSN: 2155-9570
ISSN: 2155-9570
Research Article - (2024)Volume 15, Issue 4
Objective: To compare the Choroidal Thickness (CT) in eyes with acute Central Serous Chorioretinopathy (CSC) and asymptomatic fellow eyes.
Materials and methods: A prospective, observational cross-sectional and comparative clinical study was conducted in Omani patients with acute CSC. Sub-Foveal Choroidal Thickness (SFCT) was measured manually using Enhanced Depth Imaging spectral-domain Optical Coherence Tomography (EDI-OCT) both in the affected and asymptomatic fellow eyes at presentation, 6-8 weeks and 3 months.
Results: Thirty-two eyes of sixteen patients were enrolled (16 eyes with acute CSC and 16 asymptomatic fellow eyes). The majority were males (81.3%). All patients were in their third decade of life, with a mean age of 35.75 (± 2.27 SD) years (range 30-38). The mean SFCT in eyes with acute CSC at the first, second and third visits was 426.29 (± 106.36 SD), 358.55 (± 88.66 SD), 378.98 (± 83.48) μm respectively. The mean SFCT of asymptomatic fellow eyes at the first, second and third visits was 374.08 (± 99.92 SD), 351.19 (± 93.54 SD) and 351.08 (± 55.00 SD) μm, respectively. There was no statistically significant difference in the SFCT between the first and third visit in both affected and non-affected eye groups with p-values of 0.217 and 0.073, respectively. There was no statistically significant difference between the asymptomatic fellow eyes and the affected eyes in the SFCT (P>0.05) in all visits. However, there was a trend of thicker choroid in affected eyes with around 52.21 μm differences between both eyes at the first visit.
Conclusion: This study revealed the trend of increased sub-foveal choroidal thickness at least in the initial phase of acute CSC and asymptomatic fellow eyes (affected eye>asymptomatic eye). These results support the hypothesis that CSC is a bilateral condition with an initial unilateral clinical presentation associated with a thick choroid.
Central serous chorioretinopathy; Choroid; Choroidal thickness; Pachychoroid; Optical coherence tomography; Enhanced depth imaging
CT: Choroidal Thickness; CSC: Central Serous Chorioretinopathy; SFCT: Sub-Foveal Choroidal Thickness; EDI: Enhanced Depth Imaging; OCT: Optical Coherence Tomography; EDI-OCT: Enhanced Depth Imaging Optical Coherence Tomography; SD: Standard Deviation; RPE: Retinal Pigment Epithelial; AL: Axial Length; SE: Spherical Equivalent; ACD: Anterior Chamber Depth; OCT-A: Optical Coherence Tomography Angiography; FFA: Fluorescein Angiography; ICG: Indocyanine Green angiography; VEGF: Vascular Endothelial Growth Factor; ICC: Intraclass Correlation Coefficient; IBM: International Business Machines; SPSS: Statistical Package for Social Sciences; MD: Mean Deviation; CI: Confidence Interval; SRF: Sub-Retinal Fluid; BCVA: Best Corrected Visual Acuity; NSAIDs: Non-Steroidal Anti-inflammatory Drugs
Central Serous Chorioretinopathy (CSC) is an acquired retinal condition characterized by serous retinal detachment and/or Retinal Pigment Epithelial (RPE) detachment, changes most often confined to the macula and associated with leakage of fluid through the dysfunctional RPE into the sub-retinal space (Figure 1) [1,2].
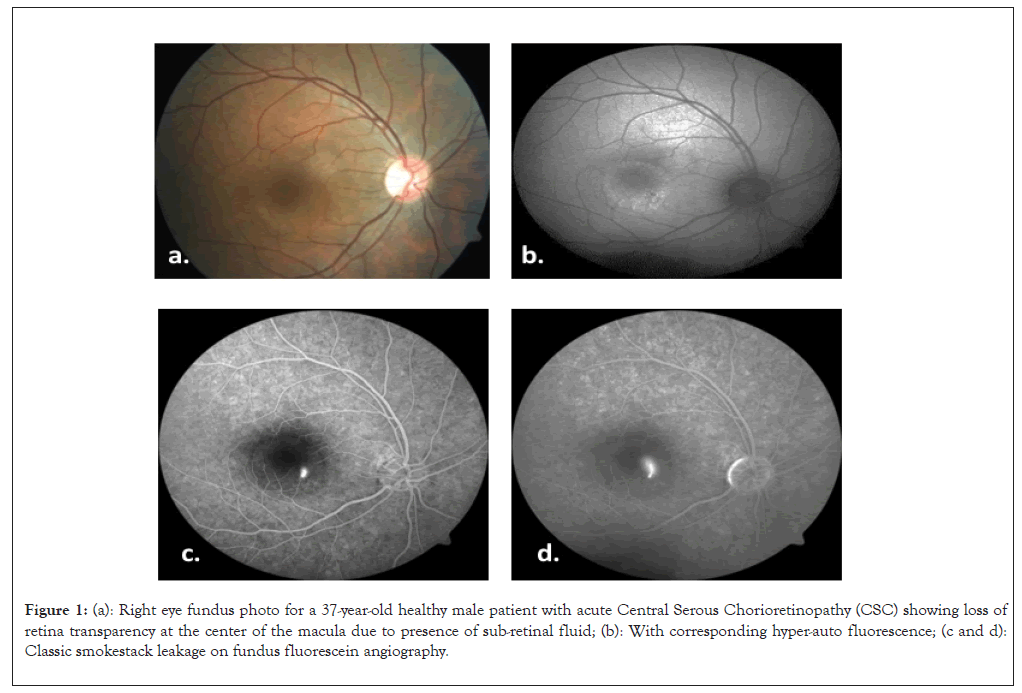
Figure 1: (a): Right eye fundus photo for a 37-year-old healthy male patient with acute Central Serous Chorioretinopathy (CSC) showing loss of retina transparency at the center of the macula due to presence of sub-retinal fluid; (b): With corresponding hyper-auto fluorescence; (c and d): Classic smokestack leakage on fundus fluorescein angiography.
CSC is relatively common retinopathy, typically affecting young to middle-aged adults [3,4]. The clinical manifestation is typically unilateral at the first visit (~ 96%) with bilateral involvement likely increasing to 20%-40% over time [5-7]. Several studies indicate that men are much more affected than women, with a male-to-female ratio of 8:1 [8].
Abnormalities of the choroidal circulation are believed to play an important role in the pathophysiology of CSC. Choroidal congestion and hyper-permeability choroidal capillaries in association with dysfunction RPE have been frequently described in this condition [9,10].
CSC is associated with multiple risk factors such as type-A personality, pregnancy, steroid usage, hypertension, H. pylori infection, sleeping disturbance, autoimmune disease, psychopharmacologic medication use and hyper-corticosteroid diseases like Cushing's syndrome [11,12]. Additionally, ocular features, such as shorter Axial Length (AL) and greater Spherical Equivalent (SE), may play a role in the pathogenesis of CSC [13].
The most common symptom of CSC is unilateral blurring of vision which initially represents as central scotoma associated with micropsia and metamorphopsia [14-16]. Chronic cases are characterized by slow deterioration in visual acuity with reduced contrast and color perception due to extensive RPE changes and secondary degenerative changes of the photoreceptors [17,18].
The Axial Length (AL) and Anterior Chamber Depth (ACD) of eyes with CSC and unaffected eyes were different in some studies, which could be related to the differences in CT and refractive error between the eyes. However, some studies showed no direct relation between CT, AL and refractive error.
A variety of imaging techniques, including Optical Coherence Tomography (OCT), Optical Coherence Tomography Angiography (OCT-A), Fluorescein Angiography (FFA) and Indocyanine Green angiography (ICG), have been utilized to diagnose and assess CSC. In this study, choroidal thickness was obtained with Enhanced Depth Imaging (EDI) mode using Heidelberg Spectralis optical coherence tomography (Heidelberg Engineering, Heidelberg, Germany) for all patients and FFA has been utilized for patients with recurrent/persistent CSC.
Quantitative analysis of the changes in the choroidal thickness might serve as useful clinical information for early diagnosis, follow-up of progression and monitoring therapeutic efficacy in eyes with CSC. At the same time, it may give useful clinical indicators about the risk of developing acute CSC in asymptomatic fellow eyes.
Normal choroidal thickness and choroidal thickness in CSC have been measured in different studies worldwide. In normal Omani adult population, sub-foveal CT was found to be 330.8 μm ± 65.5 μm which is similar to normal CT in KSA (Sub-foveal was 329.4 μm ± 56.7 μm) [19]. In Denmark population, SFCT was 342 μm ± 118 μm and in Spain SFCT was 345 μm ± 81 μm [20].
To the best of our knowledge, the study we conducted has not been carried out on Oman population before.
A prospective cohort (comparative) clinical study was conducted in the Department of Ophthalmology at Sultan Qaboos University Hospital after obtaining ethical approval from the institutional medical research ethical committee (MREC #1815) and informed consent from each patient. Patients with naive eyes with acute CSC and asymptomatic fellow eyes of the same patients were included in the study. Patients who have other ophthalmic conditions that could compromise visual acuity, choroidal thickness or quality of OCT images (e.g. corneal pathology, cataract, retinal pathology) or eyes treated previously for CSC (e.g. medically, focal laser or photodynamic therapy, Anti-Vascular Endothelial Growth Factor (VEGF), etc.) were excluded from the study.
Choroidal thickness was obtained using EDI-OCT (Heidelberg Engineering, Heidelberg, Germany) in both affected eyes and asymptomatic fellow eyes of the 16 patients with CSC. The automated segmentation of the choroidal boundaries was not a feature in the current version of software; therefore, Sub-Foveal Choroidal Thickness (SFCT) was measured manually from the outer border of the RPE-Bruch’s membrane complex to the choroid-scleral interphase at the sub-foveal area by three independent trained readers to ensure accurate CT measurements. SFCT measurements were performed at the initial presentation, 6-8 weeks and 3 months follow up visits.
Statistical analysis
Continuous variables were presented as mean and standard deviation, whereas categorical variables were presented as frequency and percentage. Comparison of means between two independent groups was carried out using the independent samples t-test, whereas the paired data were compared using the paired samples t-test. The inter-rater reliability between the three readers was assessed using the Intraclass Correlation Coefficient (ICC). A P-value less than 0.05 was considered statistically significant. All the analysis was carried out in International Business Machines (IBM) Statistical Package for Social Sciences (SPSS) version 28.0.
A total of 16 patients were enrolled (a total of 16 eyes with acute CSC and 16 asymptomatic fellow eyes). Among them, 14 (81.3%) were males and 2 (12.5) were females. All patients were in their third decade of life (mean age was 35.75 (± 2.27 SD) years, with a range 30-38 years. The following risk factors were identified; stress in 12 patients (75%), use of steroids in one patient (6%) and 3 patients (19%) had no identifiable risk factors. 31.3% were emmetropic, 37% myopic and 31% hyperopic. The mean axial length was 23.8 mm. All patients had normal anterior segment. The mean of SFCT in eyes with CSC at the first, second and third visits was 426.29 (± 106.36 SD), 358.55 (± 88.66 SD) and 378.98 (± 83.48) μm respectively. The mean of Sub Foveal Choroidal Thickness (SFCT) of the asymptomatic fellow eyes at the first, second and third visits were 374.08 (± 99.92 SD), 351.19 (± 93.54 SD) and 351.08 (± 55.00 SD) μm, respectively (Figure 2).
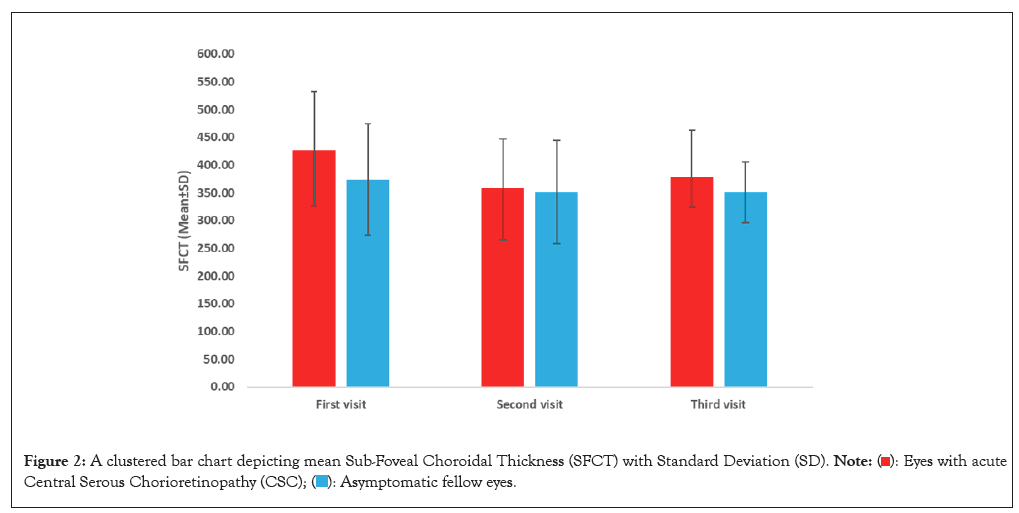
Figure 2: A clustered bar chart depicting mean Sub-Foveal Choroidal Thickness (SFCT) with Standard Deviation (SD). 

There was no statistically significant difference in the SFCT between the first visit and the third visit in the asymptomatic fellow eye group (MD=33.65, 95% CI: -3.87-71.18, P=0.073). There was no statistically significant difference in the SFCT between the first visit and third visit in eyes within the acute CSC group (MD=32.45, 95% CI: -22.86-87.76, P=0.217). Although SFCT was trending to be thicker in the CSC eyes group in comparison to the normal and asymptomatic fellow eyes, but the difference was not statistically significant (P>0.05) in all visits of the study (Table 1).
| Eyes | Mean | SD | P-value | |
|---|---|---|---|---|
| SFCT at 1st visit | Asymptomatic fellow eyes | 374.08 | 99.92 | 0.163 |
| Eyes with acute CSC | 426.29 | 106.36 | ||
| SFCT at 2nd visit | Asymptomatic fellow eyes | 351.19 | 93.54 | 0.845 |
| Eyes with acute CSC | 358.55 | 88.66 | ||
| SFCT at 3rd visit | Asymptomatic fellow eyes | 351.08 | 55.00 | 0.389 |
| Eyes with acute CSC | 378.98 | 83.48 | ||
Note: SFCT: Sub-Foveal Choroidal Thickness; CSC: Central Serous Chorioretinopathy; SD: Standard Deviation.
Table 1: Comparison between Sub-Foveal Choroidal Thickness (SFCT) in eyes with acute Central Serous Chorioretinopathy (CSC) and asymptomatic fellow eyes in all visits, (independent samples t-test, P<0.05 was considered statistically significant).
The difference between the normal mean SFCT of the Omani population and the mean CT of eyes with acute CSC (average of three visits) is 70.30 μm while the difference between the normal SFCT mean of the normal Omani population and the SFCT mean in the asymptomatic fellow eyes (average of three visits) included in this study is 31.38 μm (Table 2).
| Characteristics | Mean of normal CT in normal Omani population |
Mean CT in eyes with CSC (average of three visits) | Mean CT in asymptomatic fellow eyes (average of three visits) |
|---|---|---|---|
| SFCT | 330.8 µm | 401.10 µm | 362.18 µm |
| SD | 65.5 µm | 92.20 µm | 90.84 µm |
Note: SFCT: Sub-Foveal Choroidal Thickness; CSC: Central Serous Chorioretinopathy; SD: Standard Deviation; CT: Choroidal Thickness.
Table 2: The mean choroidal thickness of normal Omani population, eyes with Central Serous Chorioretinopathy (CSC) and asymptomatic fellow eyes.
These results support the initial hypothesis, which is that CT is more in eyes with CSC compared to asymptomatic fellow eyes as well as to the normal population eyes and CT is more in asymptomatic fellow eyes in patients with CSC compared to normal population eyes.
Inter-rater reliability analysis showed excellent agreement among the three readers for SFCT measurements, with an Intraclass Correlation Coefficient (ICC) of 0.94 (95% CI: 0.91-0.97) (Table 3).
| Group | Intraclass Correlation Coefficient (ICC) | Overall | ||
|---|---|---|---|---|
| First visit | Second visit | Third visit | ||
| Eyes with Central Serous Chorioretinopathy (CSC) | 0.917 | 0.952 | 0.762 | 0.938 |
| Asymptomatic fellow eyes | 0.936 | 0.955 | 0.791 | 0.925 |
Table 3: Inter-rater reliability test showing Sub-Foveal Choroidal Thickness (SFCT) measurements.
In this study, the authors hypothesized that there would be a difference in choroidal thickness in eyes with acute CSC compared to asymptomatic fellow eyes. However, the null hypothesis is that there is no difference.
Therefore, the authors conducted this study to compare the choroidal thickness between eyes with CSC and asymptomatic fellow eyes. The results of this study may provide further insights into the pathophysiology of CSC.
Various published literature shows that CSC is more predominant among young-middle-aged males [21,22]. Our study also evidenced the high incidence (81.3%) in young males with a mean age of 35.75 years. Like other scientific literature, our study also reveals (75% of patients) that a stressful lifestyle is a major risk factor for the development of CSC, while Haimovici, et al. [23], showed in their study 85% of patients had stress. Similar to other surveys and observations, we also noticed that any form of steroid use is well-known risk element [24].
Published scientific articles show a strong association between increased choroidal thickness and CSC [25,26]. Similarly, in our study, almost all recruited CSC patients at initial presentation showed increased sub-foveal choroidal thickness on EDI scanning with mean of 426.29 μm ± 106.36 SD, compared to 358.55 μm ± 88 SD on the second visit at 6-8 weeks in CSC eyes. This shows that choroidal thickness and CSC are positively correlated. Even in asymptomatic fellow eyes, we observed some increases in sub-foveal choroidal thickness (374.08 μm ± 99.92 SD on the first visit and 351.19 μm ± 93.54 SD on the second visit), but this gradually decreased on subsequent visits. Furthermore, comparison between the current study and previously published norms shows that the choroidal thickness values of CSC patients and their asymptomatic fellow eyes are higher than those of healthy Omani eyes (Sub-foveal choroidal thickness 330.88 μm ± 69.52 SD). CSC eyes tend to have thicker choroids compared to fellow asymptomatic eyes.
However, our study facts and figures of SFCT relatively nullify the hypothesis because they are statistically insignificant (p-value 0.217), which might be because the sample size was small. In order to validate this hypothesis, a larger sample size may be required. The natural course of acute CSC is usually self-limiting where most of the cases resolve spontaneously within 3 months from the onset in about 70% to 80% of cases with a recurrence rate of 50% within a year [27]. However, persistent CSC in which clinical findings last beyond 4 to 6 months can result in progressive RPE atrophy and permanent visual loss and treatment is warranted for such cases to prevent permanent visual loss [28,29].
Out of 16 eyes in this study, three eyes (of three patients) had persistent CSC since initial presentation and through follow-up visits. The first patient stopped following up after the third visit and the second patient remained symptomatic on subsequent visits after the study period. While the third patient developed a recurrence between 4 and 5 months after the initial presentation. Two patients were treated with FFA-guided green focal laser photocoagulation. Both patients had complete resolution of Sub-Retinal Fluid (SRF) and vision was restored to 20/20, but they developed paracentral scotomas caused by changes in RPE and ellipsoid zone. Focal laser photocoagulation is one of the treatment options for persistent or recurrent CSC which shows its effectiveness in this study. Furthermore, Sangal, et al. [29], found in their case series that focal laser photocoagulation can further improve vision and resolve SRF in cases of persistent and recurrent CSC (Figure 3).
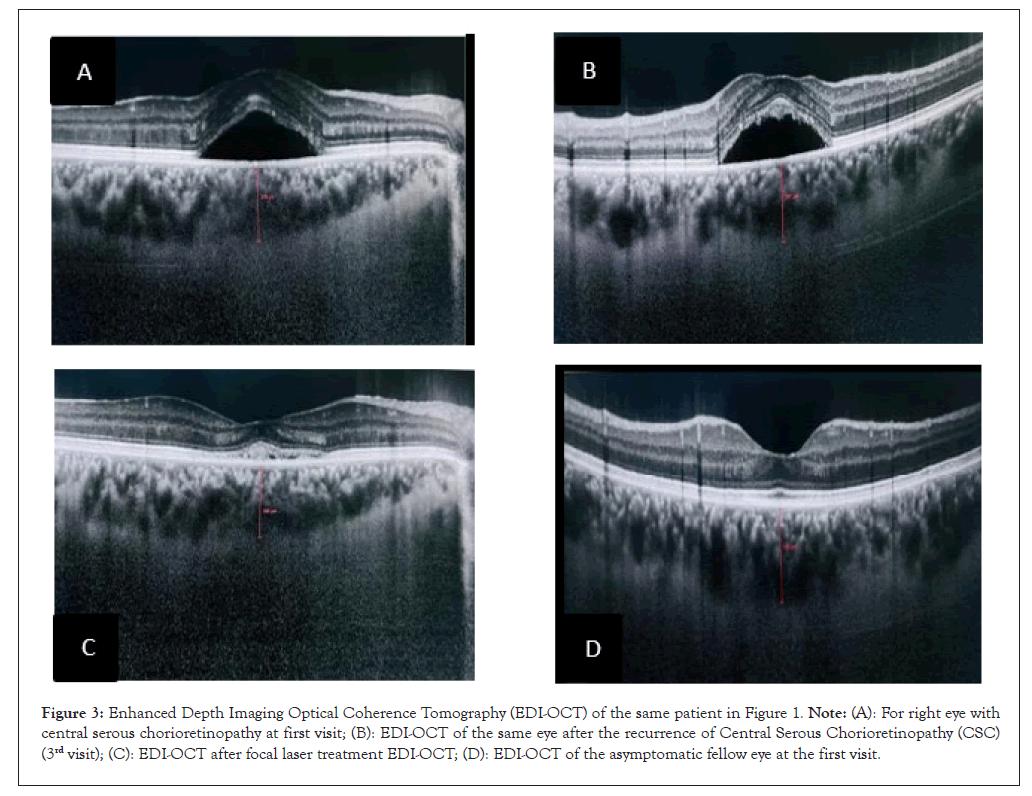
Figure 3: Enhanced Depth Imaging Optical Coherence Tomography (EDI-OCT) of the same patient in Figure 1. Note: (A): For right eye with central serous chorioretinopathy at first visit; (B): EDI-OCT of the same eye after the recurrence of Central Serous Chorioretinopathy (CSC) (3rd visit); (C): EDI-OCT after focal laser treatment EDI-OCT; (D): EDI-OCT of the asymptomatic fellow eye at the first visit.
Multiple other treatment modalities have been established to treat persistent or recurrent CSC. Half-fluence photodynamic therapy with verteporfin and subthreshold micro-pulse laser treatment have shown the most promising results [30-32]. Moreover, there have been new insights into multiple medical therapies, such as trials of oral eplerenone being done which have shown controversies. However, some studies have shown that eplerenone improves vision and has a good efficacy in treating blindness [33,34]. Whereas VICI-randomized multicenter trial in the UK showed eplerenone is not superior to placebo for improving Best Corrected Visual Acuity (BCVA) in chronic CSC after a year [35].
Numerous other trials of pharmacotherapy have been carried out and shown inconsistent outcomes including the use of topical Non-Steroidal Anti-inflammatory Drugs (NSAIDs), oral propranolol, Spironolactone and topical carbonic anhydrase inhibitor (dorzolamide) [36]. There is no clear evidence of the efficacy of intravitreal anti-vascular endothelial growth factor therapy in chronic CSC. Finally, the inter-rater reliability analysis in our study showed an excellent agreement among the three readers for SFCT measurements, with an Intraclass Correlation Coefficient (ICC) value of 0.94. This indicates that the manual measurement method used was reliable and reproducible, enhancing the validity of our findings.
Despite the small sample size, this study has confirmed the previously published observation of increased CT in both eyes with symptomatic CSC and asymptomatic fellow eyes in comparison to normal population. This observation supports the hypothesis that CSC is a bilateral condition with initial unilateral clinical presentation. Moreover, CT can be used as OCT biomarker for evaluating patients with acquired maculopathies. Further studies with larger sample size and longer follow-up periods might be useful to validate such observations and to evaluate the long-term changes in CT in eyes with the spontaneously resolved/treated/ recurrent CSC and the risk of developing acute CSC in the asymptomatic fellow eyes.
We would like to thank the following colleagues: Mrs. Hanan Al Harthi and Ms. Sadika Al-Ajmi Ophthalmic technicians, Mr. Harith Al-Hasani, Optometrist, Department of Ophthalmology, Sultan Qaboos University Hospital for assisting in performing the diagnostic tests and Mr. Sachin Jose and Mr. Sathyia Murthi, Statistics Specialists, Research Section, Oman Medical Specialty Board for assisting in data analysis.
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
Citation: Al-Aliyani A, Al-Abri M, Al-Hinai A, Al-Fadhil N, Mal W (2024) Comparison of Choroidal Thickness in Acute Central Serous Chorioretinopathy and Asymptomatic Fellow Eyes in the Omani Population. J Clin Exp Ophthalmol. 15:981.
Received: 03-Jun-2024, Manuscript No. JCEO-24-31556; Editor assigned: 05-Jun-2024, Pre QC No. JCEO-24-31556 (PQ); Reviewed: 19-Jun-2024, QC No. JCEO-24-31556; Revised: 26-Jun-2024, Manuscript No. JCEO-24-31556 (R); Published: 04-Jul-2024 , DOI: 10.35248/2155-9570.24.15.981
Copyright: © 2024 Al-Aliyani A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.